Ultrasound-guided cystocentesis represents a significant advancement in veterinary medicine, offering real-time visualization for safer and more accurate urinary bladder access․
What is Cystocentesis?
Cystocentesis is a minimally invasive procedure involving the percutaneous placement of a needle into the urinary bladder to collect a sterile urine sample․ Traditionally performed by palpation, it’s crucial for diagnosing urinary tract infections and assessing bladder health․ However, relying solely on palpation can be challenging, especially in obese patients or those with a small, deeply-seated bladder․ This technique bypasses contamination from the urethra, providing a clean sample for accurate analysis․ It’s a common diagnostic tool in veterinary medicine, offering valuable insights into a patient’s urinary system function․
The Role of Ultrasound Guidance
Ultrasound guidance dramatically improves the accuracy and safety of cystocentesis․ Real-time visualization allows precise needle placement, avoiding abdominal vasculature and other critical structures․ This is particularly beneficial in challenging cases where palpation is unreliable․ Ultrasound also aids in identifying the optimal puncture site, assessing bladder wall thickness, and detecting potential abnormalities like stones or masses․ Consequently, ultrasound-guided cystocentesis minimizes the risk of complications, such as hematuria or bladder perforation, leading to a more confident and effective procedure․

Indications for Ultrasound-Guided Cystocentesis
Ultrasound guidance is indicated for urinary retention, obstruction, suspected urinary tract infections, and assessment of bladder masses, enhancing diagnostic accuracy and safety․
Urinary Retention
Ultrasound-guided cystocentesis is particularly valuable when dealing with urinary retention, especially when the cause isn’t immediately clear․ It allows for direct visualization of the bladder, confirming distension and ruling out obstructions like urethral blockages or bladder stones contributing to the inability to urinate․
This technique ensures accurate needle placement, minimizing trauma and maximizing urine sample collection even in a severely distended, yet potentially fragile, bladder․ It’s a crucial diagnostic and therapeutic step․
Urinary Obstruction
Ultrasound-guided cystocentesis plays a vital role in managing urinary obstruction cases, aiding in both diagnosis and temporary relief․ Ultrasound can identify the location and nature of the obstruction – whether it’s a urethral stricture, bladder stone, or mass – guiding subsequent treatment plans;
While not resolving the obstruction itself, cystocentesis provides immediate decompression, alleviating patient discomfort and preventing further bladder damage until definitive intervention is possible․
Diagnosis of Urinary Tract Infections
Ultrasound-guided cystocentesis is invaluable for obtaining a sterile urine sample for culture and sensitivity, crucial for diagnosing urinary tract infections (UTIs)․ The ultrasound guidance ensures accurate needle placement directly into the bladder, minimizing contamination from the urethra or perineal skin․
This technique is particularly beneficial in patients where obtaining a urine sample via traditional methods is challenging or unreliable, leading to a more accurate diagnosis and targeted antibiotic therapy․
Assessment of Bladder Masses
Ultrasound-guided cystocentesis aids in the assessment of potential bladder masses by allowing for simultaneous visualization of the mass and sterile urine sample collection․ This is critical for cytology, helping differentiate between inflammatory, benign, and malignant processes within the bladder wall․
Ultrasound can characterize the mass’s appearance, size, and location, guiding further diagnostic steps like biopsy or surgical planning, improving diagnostic accuracy and treatment strategies․

Pre-Procedure Preparation
Thorough preparation involves a complete patient history, physical exam, informed consent, and a meticulously checked equipment list for optimal outcomes․
Patient History and Physical Examination
A detailed patient history is crucial, focusing on prior urinary issues, current medications (especially those affecting coagulation), and any relevant underlying conditions․ The physical examination should assess hydration status, abdominal palpation for bladder distension or pain, and overall systemic health․
Specifically, evaluate for signs of urinary tract infection, like abdominal discomfort or straining to urinate․ Document any abnormalities thoroughly, as these findings will directly influence procedural planning and interpretation of ultrasound images․ A complete assessment minimizes risks and maximizes diagnostic yield․
Informed Consent
Obtaining informed consent is paramount before proceeding with ultrasound-guided cystocentesis․ Owners must understand the procedure’s purpose, benefits, and potential risks – including hematuria, urine leakage, infection, and, rarely, bladder perforation․
Clearly explain alternative diagnostic options and the implications of declining the procedure․ Document the discussion, addressing owner questions and ensuring they acknowledge understanding and voluntarily consent to the cystocentesis․ A signed consent form is essential for legal and ethical practice․
Equipment Checklist
A comprehensive equipment checklist is crucial for a smooth ultrasound-guided cystocentesis․ Essential items include an ultrasound machine with appropriate probe, sterile gloves, surgical prep solution (chlorhexidine), local anesthetic (lidocaine), a sterile urinary collection system (syringe and needle or catheter), and sterile drapes․
Additional necessities are gauze, cotton balls, and appropriate personal protective equipment․ Ensure all equipment is functioning correctly before beginning the procedure to avoid delays or complications․
Ultrasound Technique
Effective ultrasound technique involves selecting the correct probe, identifying the bladder, assessing fluid volume, and visualizing anatomical landmarks for safe needle guidance․
Probe Selection and Frequency
Choosing the appropriate ultrasound probe is crucial for optimal visualization during cystocentesis․ A curvilinear probe, typically with a frequency range of 5-9 MHz, is often preferred due to its wider field of view and deeper penetration․
Higher frequency probes (e․g․, 7-12 MHz) offer improved resolution for superficial structures but may not penetrate as deeply in larger patients․ Conversely, lower frequencies enhance penetration in obese individuals․ Adjusting the frequency dynamically during the scan can optimize image quality based on patient size and anatomy, ensuring accurate bladder assessment․
Bladder Identification and Measurement
Locating the urinary bladder on ultrasound involves a systematic approach, scanning from the abdominal midline caudally; The bladder appears as a fluid-filled, anechoic (black) structure․ Accurate measurement of bladder length, width, and height is essential for assessing urine volume and identifying potential abnormalities․
Documenting these dimensions provides a baseline for monitoring and helps determine the optimal needle insertion site, avoiding vasculature and other critical structures during cystocentesis․
Fluid Assessment within the Bladder
Ultrasound allows for detailed assessment of the fluid characteristics within the bladder․ Homogeneous, anechoic fluid is typical of normal urine․ However, the presence of sediment, echogenic debris, or layering suggests inflammation, infection, or the presence of stones․
Evaluating fluid echogenicity guides clinical decisions and helps differentiate between various urinary tract pathologies before needle insertion, improving diagnostic accuracy during cystocentesis․
Procedure Steps
Guided by ultrasound, cystocentesis involves aseptic preparation, local anesthesia, careful needle advancement, and controlled urine collection for diagnostic purposes․
Aseptic Preparation
Meticulous aseptic technique is paramount during ultrasound-guided cystocentesis to minimize the risk of introducing infection into the urinary bladder․ The area over the urinary bladder, identified via ultrasound, should be clipped of hair and aseptically scrubbed with a chlorhexidine solution․
This is followed by surgical preparation with an alcohol solution, allowing it to dry completely before proceeding․ Sterile drapes are then applied to create a sterile field, isolating the intended puncture site and maintaining a sterile environment throughout the procedure․
Local Anesthesia
Local anesthesia is crucial for patient comfort during ultrasound-guided cystocentesis․ Following aseptic preparation, a small amount of local anesthetic, typically lidocaine or bupivacaine, is infiltrated subcutaneously at and around the planned needle insertion site․
Ultrasound guidance can assist in visualizing the anesthetic spread, ensuring adequate coverage of the tissues․ Gentle pressure should be applied after injection to further distribute the anesthetic, minimizing discomfort upon needle advancement․
Needle Insertion and Advancement
Needle insertion should be performed with a smooth, confident motion, maintaining continuous visualization via ultrasound․ The needle is advanced under real-time guidance, aiming for the cranial aspect of the bladder, avoiding any visible vessels or organs․
A slight “pop” may be felt as the needle penetrates the bladder wall․ Continuous monitoring of the needle tip’s position is vital to prevent inadvertent trauma to surrounding structures, ensuring a safe and accurate procedure․
Urine Collection
Once the needle is within the bladder lumen, a syringe is attached to gently aspirate urine․ Avoid vigorous suction, as this can cause bladder spasms or trauma․ The amount of urine collected should be sufficient for diagnostic testing, typically 5-10ml․
Observe the urine’s color and clarity during collection․ After collection, the needle is swiftly removed, and gentle pressure is applied to the puncture site to minimize bleeding or leakage․

Post-Procedure Care
Following cystocentesis, careful monitoring for complications like hematuria is crucial, alongside appropriate fluid therapy and continued bladder assessment protocols․
Monitoring for Complications
Post-procedure observation is paramount, focusing on identifying potential issues promptly․ Closely monitor the urinary catheter site for any signs of bleeding, swelling, or discharge․ Assess the patient for hematuria – blood in the urine – which is relatively common but requires tracking․
Vigilance for urine leakage around the cystocentesis site is also essential․ Regularly evaluate the patient’s overall condition, including vital signs, to detect early indicators of infection or other adverse reactions․ Prompt intervention can mitigate complications and ensure a favorable outcome․
Fluid Therapy
Following cystocentesis, fluid therapy may be indicated based on the patient’s hydration status and any pre-existing conditions․ Intravenous fluids can help maintain adequate renal perfusion and support overall circulatory volume, particularly if the patient was previously dehydrated․
The type and rate of fluid administration should be tailored to the individual patient’s needs, considering factors like age, weight, and concurrent illnesses․ Careful monitoring of fluid balance is crucial to prevent overhydration or electrolyte imbalances․
Bladder Monitoring
Post-cystocentesis, regular bladder monitoring is essential to assess for complications like hematuria or urine leakage․ Ultrasound can be repeated to evaluate bladder wall integrity and confirm complete urine drainage․ Frequent observation of the patient’s urination habits is also crucial․
Monitoring helps detect any signs of discomfort or difficulty urinating, allowing for prompt intervention if needed․ Documenting urine volume and appearance provides valuable information regarding bladder function and recovery․

Potential Complications
Although generally safe, ultrasound-guided cystocentesis carries risks including hematuria, urine leakage, infection, and, rarely, bladder perforation requiring immediate attention․
Hematuria
Hematuria, or the presence of blood in the urine, is a relatively common post-cystocentesis finding․ Typically, it’s mild and self-limiting, resolving within 24-48 hours as the bladder heals; The ultrasound guidance minimizes trauma to bladder vasculature, reducing the incidence and severity․ However, significant or persistent hematuria warrants further investigation to rule out underlying bladder pathology or iatrogenic injury․ Monitoring urine color and volume is crucial, and supportive care, including fluid therapy, may be indicated in severe cases․
Urine Leakage
Urine leakage following ultrasound-guided cystocentesis is an infrequent, yet concerning, complication․ It usually stems from a small bladder perforation, though it can also occur if the needle tract doesn’t adequately seal post-procedure․ Ultrasound can help identify potential leakage sites․ Management involves strict cage rest, fluid restriction, and close monitoring; In some instances, a urinary catheter may be necessary to divert urine and allow the bladder to heal․ Prompt recognition and intervention are vital to prevent further complications․
Infection
Infection, though rare with meticulous technique, remains a potential complication of ultrasound-guided cystocentesis․ Strict aseptic preparation is paramount to minimize bacterial introduction․ Post-procedure monitoring for signs like fever, dysuria, or pyuria is crucial․ If infection is suspected, urine culture and sensitivity testing should be performed to guide antibiotic therapy․ Prophylactic antibiotics are generally not recommended, but may be considered in high-risk patients․
Bladder Perforation (Rare)
Bladder perforation is an uncommon, yet serious, complication of ultrasound-guided cystocentesis․ Careful needle advancement under continuous ultrasound visualization is essential to avoid inadvertent penetration of the bladder wall․ If perforation occurs, immediate recognition is vital, often indicated by leakage of urine outside the bladder lumen․ Surgical intervention may be required for larger perforations, while smaller ones can sometimes be managed conservatively with fluid therapy and monitoring․
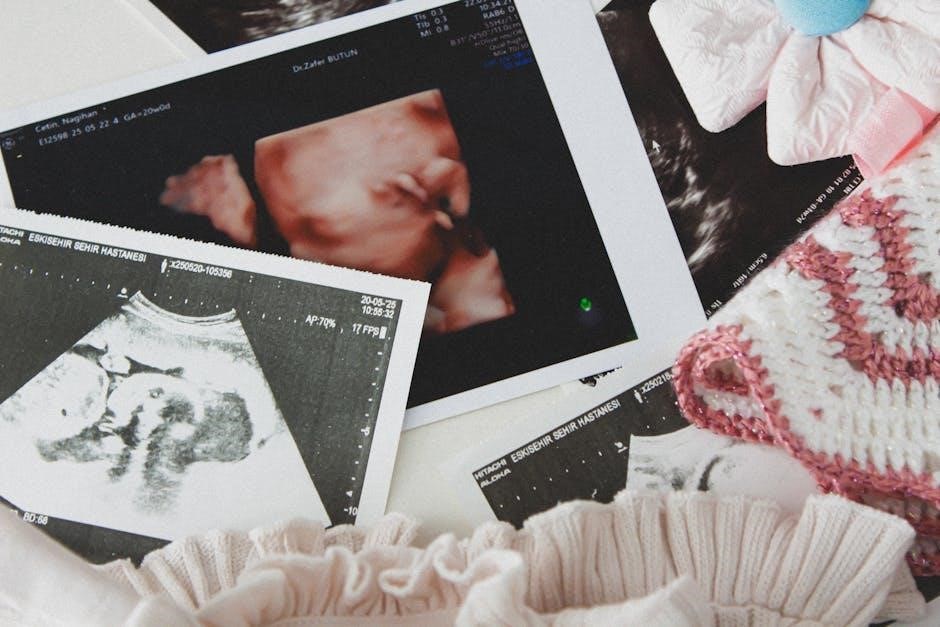
Ultrasound Findings & Interpretation
Ultrasound reveals bladder wall thickness, stones, and hydroureter, aiding accurate cystocentesis․ Proper interpretation guides needle placement, minimizing risks and maximizing diagnostic yield․
Identifying Bladder Wall Thickness
Assessing bladder wall thickness via ultrasound is crucial for diagnosing various conditions․ A normal bladder wall typically measures between 2-3mm when distended․ Increased thickness can indicate cystitis, edema, or even a mass lesion within the bladder wall itself․ Ultrasound allows differentiation between mucosal and muscular layer thickening․
Careful measurement, utilizing standardized techniques, is essential for accurate interpretation․ Comparing measurements to previous scans, if available, provides valuable insight into disease progression or response to treatment․ Experienced sonographers can readily identify subtle changes indicative of underlying pathology․
Detecting Bladder Stones
Ultrasound excels at identifying bladder stones, often appearing as hyperechoic (bright) foci within the urinary bladder lumen․ A key characteristic is their acoustic shadowing – a dark area behind the stone due to sound wave blockage․ This differentiates them from sediment․
Ultrasound can determine stone size, number, and location, guiding treatment decisions․ Mobile stones shift with patient positioning, while fixed stones may indicate impaction․ Doppler can assess blood flow around the stones, revealing potential inflammation․
Assessing for Hydroureter
Ultrasound is crucial for detecting hydroureter – dilation of the ureters – often indicating urinary obstruction․ The ureters appear as anechoic (dark) tubular structures extending from the renal pelvis to the bladder․ Increased ureteral diameter suggests backflow pressure․
Evaluating the degree of dilation helps determine the severity of obstruction․ Doppler assessment can reveal absent or diminished blood flow within the ureteral walls, further supporting obstruction․ This finding guides immediate intervention strategies․

Variations in Technique
Techniques vary, including freehand approaches and utilizing ultrasound elastography to assess bladder wall properties and potentially identify subtle abnormalities․
Freehand Ultrasound-Guided Cystocentesis
Freehand technique involves skilled visualization and manual needle guidance, relying on the operator’s experience to correlate ultrasound images with anatomical landmarks․ This method requires a steady hand and precise coordination, offering flexibility without specialized equipment․ Real-time ultrasound allows for dynamic adjustments during needle advancement, minimizing the risk of vascular or organ puncture․ However, it demands significant operator proficiency to maintain accuracy and safety, particularly in challenging anatomical situations or with uncooperative patients․ Careful probe stabilization is crucial for consistent imaging․
Using Ultrasound Elastography
Ultrasound elastography is an emerging technique that assesses tissue stiffness, potentially aiding in bladder mass characterization during cystocentesis․ By visualizing tissue elasticity, it can differentiate between benign and malignant lesions, guiding targeted sampling․ This advanced imaging modality provides quantitative data beyond conventional ultrasound, enhancing diagnostic accuracy․ While still under investigation for cystocentesis specifically, elastography holds promise for improved lesion assessment and minimizing unnecessary biopsies․ Further research is needed to establish its clinical utility and refine interpretation criteria․
Cystocentesis in Specific Populations
Ultrasound guidance adapts cystocentesis for diverse patients – pediatric, geriatric, and obese – ensuring accurate bladder access and minimizing potential complications․
Pediatric Patients
Performing cystocentesis in pediatric patients requires meticulous technique due to their smaller bladder size and delicate anatomy․ Ultrasound guidance is particularly crucial, allowing precise needle placement and reducing the risk of inadvertent organ puncture․ Careful probe selection, utilizing higher frequency transducers, enhances visualization of the bladder wall and surrounding structures․
Real-time imaging confirms appropriate needle trajectory and depth, minimizing trauma and discomfort․ Maintaining patient stability and employing gentle restraint are also paramount considerations when performing this procedure in young animals․
Geriatric Patients
Ultrasound-guided cystocentesis offers significant benefits in geriatric patients, who often present with decreased bladder elasticity and potential underlying conditions․ Age-related changes can make traditional palpation-guided techniques less reliable and increase the risk of complications․ Ultrasound allows for accurate assessment of bladder wall thickness and the presence of masses or stones․
Gentle technique and careful monitoring are essential, as geriatric patients may have compromised renal function or concurrent medical issues․ Ultrasound ensures safe and effective urine collection․
Patients with Obesity
Obese patients often present challenges for traditional cystocentesis due to increased subcutaneous fat, making bladder palpation difficult․ Ultrasound guidance overcomes this limitation by providing direct visualization of the urinary bladder, regardless of body condition score․ Accurate probe positioning and frequency adjustment are crucial for optimal image quality․
Careful consideration should be given to needle length to ensure adequate penetration through adipose tissue, minimizing the risk of incomplete bladder aspiration or trauma to surrounding structures․

Comparison to Traditional Cystocentesis
Ultrasound guidance demonstrably improves accuracy and safety during cystocentesis, significantly reducing the incidence of complications compared to palpation-based techniques․
Accuracy and Safety
Ultrasound guidance elevates the precision of cystocentesis by providing direct visualization of the urinary bladder, its contents, and surrounding structures․ This real-time imaging minimizes the risk of accidental puncture of adjacent organs, like the intestines․ Traditional cystocentesis relies heavily on palpation, which can be unreliable, especially in obese patients or those with unusual anatomical configurations․ Consequently, ultrasound significantly enhances procedural safety and diagnostic yield, leading to fewer failed attempts and reduced patient discomfort․ It allows for targeted needle placement, improving sample quality․
Reduced Risk of Complications
Employing ultrasound guidance during cystocentesis demonstrably lowers the incidence of common complications․ The precise visualization minimizes hematuria, urine leakage, and the potential for inadvertent bladder perforation․ By avoiding blind needle insertion, the risk of intestinal or vascular trauma is substantially decreased․ This technique is particularly beneficial in patients with challenging anatomy or those predisposed to bleeding․ Overall, ultrasound-guided cystocentesis offers a safer alternative, promoting improved patient outcomes and minimizing post-procedural morbidity․
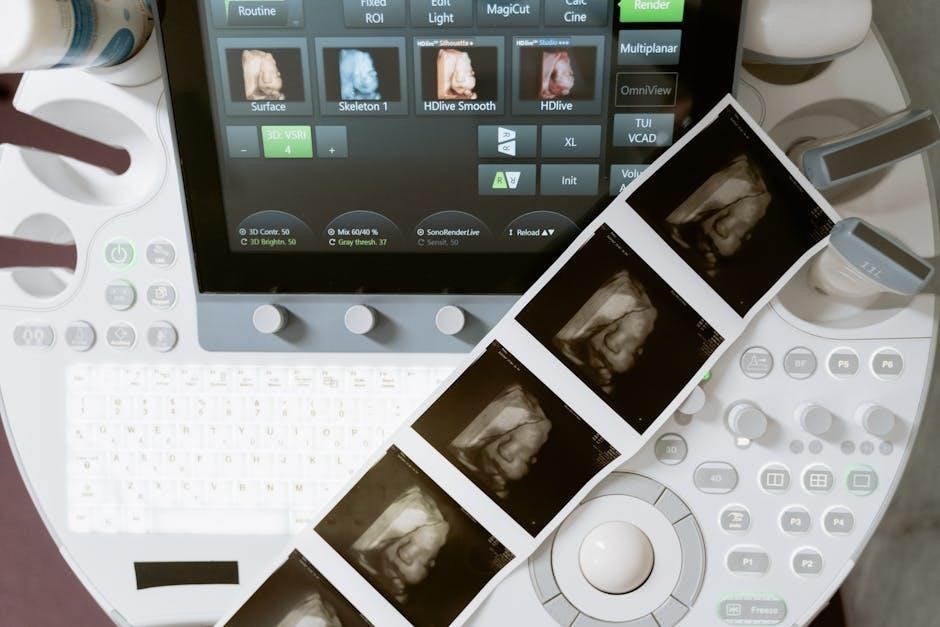
Future Directions in Ultrasound-Guided Cystocentesis
Innovations like contrast-enhanced ultrasound and artificial intelligence promise to further refine accuracy, streamline workflows, and enhance diagnostic capabilities in cystocentesis․
Contrast-Enhanced Ultrasound
Contrast-enhanced ultrasound (CEUS) utilizes microbubble contrast agents injected intravenously to amplify ultrasound signals, improving visualization of bladder wall vasculature and subtle lesions․ This technique can differentiate between benign and malignant bladder masses with greater precision during cystocentesis․ CEUS aids in identifying areas of neovascularity, indicative of tumor growth, and can help guide targeted biopsies․ Furthermore, it enhances the detection of bladder wall thickening or irregularities, potentially revealing early signs of inflammation or disease that might otherwise be missed;
Artificial Intelligence Assistance
Artificial intelligence (AI) is poised to revolutionize ultrasound-guided cystocentesis by automating image analysis and enhancing diagnostic accuracy․ AI algorithms can be trained to automatically identify the bladder, measure its dimensions, and detect abnormalities like stones or masses․ Real-time AI assistance can guide needle placement, minimizing the risk of complications․ Furthermore, AI can standardize image interpretation, reducing inter-observer variability and improving the efficiency of the procedure, ultimately leading to better patient outcomes․
Ultrasound guidance significantly improves cystocentesis safety and accuracy, offering benefits like reduced complications and enhanced visualization for optimal bladder access and fluid collection․
Benefits of Ultrasound Guidance
Employing ultrasound during cystocentesis delivers numerous advantages over traditional palpation-guided techniques․ Real-time imaging allows precise needle placement, minimizing the risk of encountering unseen vasculature or intestinal loops․ This leads to decreased hematuria and urine leakage post-procedure․
Furthermore, ultrasound aids in identifying the optimal puncture site, especially in patients with obesity or a distended abdomen where palpation is unreliable․ It also confirms adequate bladder filling and helps differentiate between urine and other abdominal contents, enhancing diagnostic accuracy․
Importance of Proper Technique
Mastering ultrasound-guided cystocentesis necessitates meticulous attention to detail․ Correct probe selection and frequency adjustment are crucial for optimal bladder visualization․ A systematic approach to scanning, including accurate bladder measurement and fluid assessment, is paramount․
Aseptic preparation and appropriate local anesthesia minimize patient discomfort and infection risk․ Controlled needle advancement, guided by real-time imaging, prevents inadvertent trauma․ Consistent practice and adherence to established protocols are essential for maximizing safety and efficacy․